
Next steps:
Feel free to read the advice sheet below! To get the full benefit click on 'Start treatment'. By starting the treatment you will get access to weekly rehab programmes online for FREE. You will be able to track your progress, pain levels and we will remind you to do your exercises every day!
Osteoarthritis (OA) is commonly referred to as wear and tear arthritis, which is a condition where the natural cushioning between the joints wears away. Whenever this happens, the bones within the joint end up rubbing closely together with less of the benefits commonly found in the cartilage relating to shock-absorbing. The rubbing of the joints together ends up causing swelling, pain, stiffness and a decreased ability to move, as well as the formation of bone spurs.
Even though age is a major risk factor contributing to osteoarthritis of the knee, younger individuals can get it as well. For some individuals, osteoarthritis might be hereditary. For others, the condition can result from infection or an injury to the knee, as well as being overweight.
Osteoarthritis is the most common of all forms of arthritis. Even though it can occur in younger individuals, the chance of developing the condition increases after the age of 45. More than 27 million Americans are affected with the condition, with the knee as one of the most commonly affected areas. Women tend to be more prone to the condition than men.
But What Exactly Happens During Knee OA in Simple Terms?
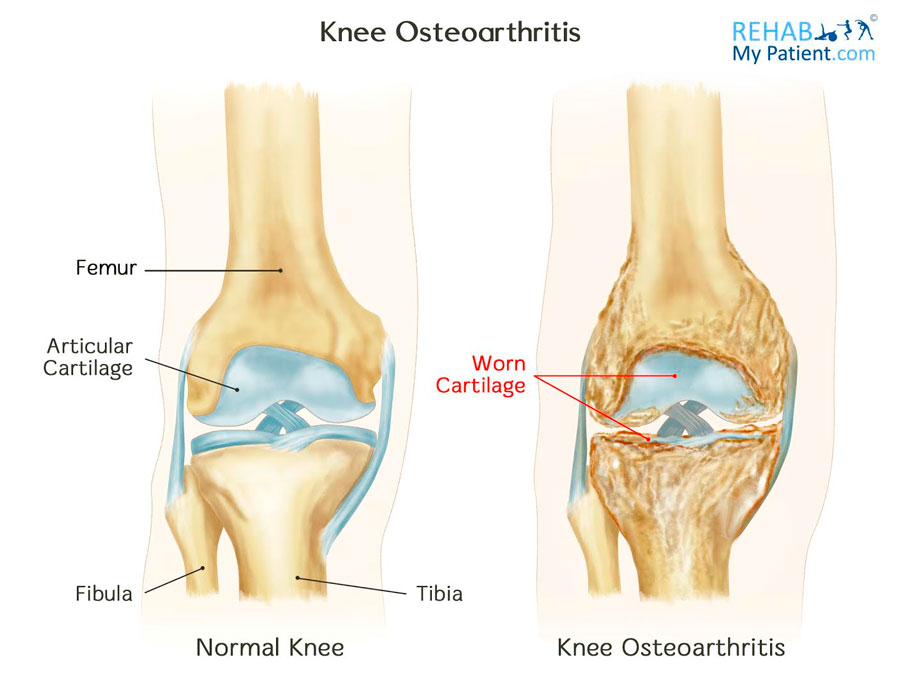
Usually due to wear and tear, or an injury to the joint, the protective cartilage around the knee gets worn or damaged. When this cartilage wears out, you have bone on bone without any cartilage to protect the underlying bone. This causes inflammation along the joint line. The body tries to protect the area by laying down bone, and the joint enlarges. Osteophytes (rogue growths of bone) form, and the capsule around the joint thickens. This causes gross stiffness, swelling and pain. As the condition worsens, the sufferer naturally looks to medical help which may include therapy, drugs, or surgery.
Knee Osteoarthritis Anatomy
The knee is one of the biggest and most complex of all joints found in the body. It joins the shin bone and the thigh bone together. The smaller bone running alongside of the tibia and the kneecap are the two other bones that complete the knee joint. Tendons keep the leg muscles and knee bones connected to enable the knee joint to move. Ligaments join all of the knee bones and deliver stability to the knee.
The anterior cruciate ligament is the one that prevents the femur from sliding backward along the tibia. The medial and lateral collateral ligaments make sure the femur doesn’t slide from one side to the other. It is the posterior cruciate ligament that prevents the femur from sliding forward along the tibia.
Sitting on the edge of the bones is cartilage, and above the cartilage is a C-shaped structure called a meniscus. This meniscus is a shock-absorber to the knee, and can be torn during twisting injuries and sports injuries. Tears to the meniscus predispose the patient to knee OA.
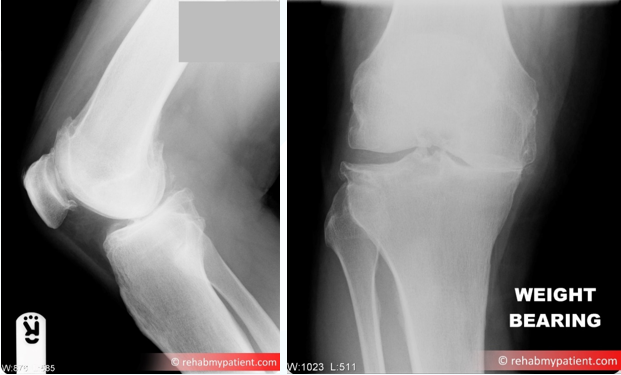
X-ray showing knee osteoarthritis
How to Treat Knee Osteoarthritis:
- Weight Loss
Losing even a small amount of weight can reduce the pain from osteoarthritis significantly.
- Exercise
Strengthening the muscles surrounding the knee will make the joint more stable and help to decrease the pain. Stretching exercises keep the knee joint more flexible and mobile. The true key is to get as much movement as you can to the knee joint, and this tends to reduce the inflammation and pain.
- Corticosteroids
Steroids tend to be one of the most powerful anti-inflammatory drugs around, which helps to reduce swelling and pain in the joint.
- Braces
Unloader braces help take the weight away from the affected side of the knee, while support braces provide you with support for the entire knee. They can be used when the knee is under pressure or strain and usually are used for the short-term.
- Surgery
The first defense is usually an arthroscopy (known as keyhole surgery) where the surgeon will “wash-out” or clean out the joint. Basically the surgeon will look inside the knee, work out what parts of the knee are causing the pain, and then remove, trim, or stitch the offending parts. However, if the arthritis in the knee is more extensive, sometimes knee arthroscopies are not likely to be successful, so a more substantial surgery is needed. The first step may be a half knee replacement, replacing the side which is most affected (assuming one side is a lot worse than the other side), or total knee replacement where the whole joint is replaced with an implant. See the advice sheet on knee replacement.
Tips:
- As you grow older, the ability of your cartilage to heal tends to decrease.
- Every pound of weight gained will add an additional three to four pounds of weight on the knees, so the best thing you can do is to maintain a healthy weight.
- Certain occupations that involve repeated activity stressing the joint, such as squatting, lifting heavy objects and kneeling, cause individuals to develop the condition due to the constant pressure on the joint.
- Athletes participating in tennis, soccer or long-distance running are at an increased risk of developing the condition.
- For those who have certain metabolic disorders, the risk of developing osteoarthritis increases.

